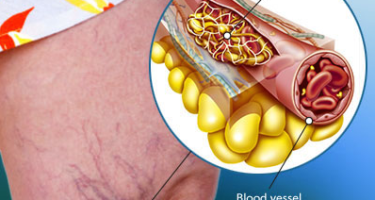
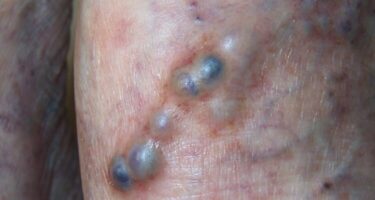
Orthopedics Atherosclerosis is a condition where plaque builds up inside your arteries. This can lead to blockages and reduce blood flow to your legs. You may also experience pain or discomfort in your legs. Your doctor may recommend treatment if you have symptoms.
TREATMENT FOR PATIENTS IN OKEECHOBEE WITH ARTERIAL DISEASE
What are the main causes of peripheral arterial disease for patients in Okeechobee Florida to seek treatment options at Symmetry Vascular Surgery.

ARTERIAL VASCULAR DISEASE TREATMENT FOR PATIENTS IN OKEECHOBEE FLORIDA
SYMMETRY VASCULAR CENTER is proud to offer a complete range of services for patients suffering from peripheral arterial disease.
We treat patients with lower extremity peripheral arterial disease (PAD) who live in Okeechobee Florida.
For patients in Okeechobee suffering from peripheral arterial disease, Symmetry Vascular Center offers a comprehensive range of vascular surgery services. In addition to in-office consultation, we offer surgery for patients with peripheral arterial disease and chronic venous disease. By performing many of these procedures in this setting, we deliver an unparalleled patient experience with cutting-edge technology.
PAD is caused by atherosclerosis or hardening of the arteries. Atherosclerotic plaques block the blood flow through the arteries, causing reduced blood flow and nutrients to your legs. There are three common conditions that result in treatment plans.
1. Ulceration / Gangrene
Ulcers on your toes and/or feet. These can last for months without healing. Severely damaged circulation may lead to ulcers with no oxygen or nutrients to form healthy tissue. In extreme cases, these can lead to infection and gangrene. A prompt evaluation by the vascular surgery team can help alleviate the problem and put you at ease.
2. Rest Pain
A burning or throbbing feeling in your foot, often worse at nighttime when trying to sleep. Often this is a sign of impending, irreversible damage to your leg. A referral to the vascular surgery team is important because they can perform a proper workup and determine if surgery is needed.
3. Claudication
A cramping sensation in your buttocks, thighs, or calf muscles. Treatments include medical therapy, lifestyle changes, smoking cessation, exercise and, in rare circumstances surgery.
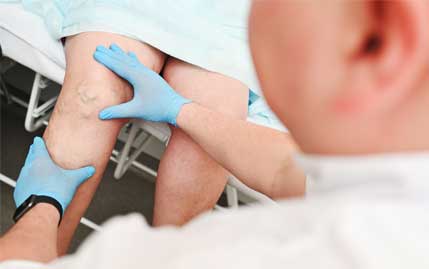
SYMMETRY VASCULAR CENTER IS PROUD TO OFFER TREATMENT FOR PATIENTS WITH VASCULAR ARTERIAL DISEASE IN OKEECHOBEE FLORIDA
SYMMETRY VASCULAR CENTER IS PROUD TO OFFER TREATMENT FOR PATIENTS WITH ARTERIAL DISEASE LOCATED IN OKEECHOBEE FLORIDA
Symmetry Vascular Center Doctors & Staff
The team at Symmetry Vascular Center is dedicated to delivering cutting-edge, vascular care to the Treasure Coast community. Our Board-Eligible/Board-Certified physicians and Advanced Practice Providers are proud to provide care in our Office, Cleveland Clinic Martin Health, and St. Lucie Medical Center.
What Are Varicose Veins?
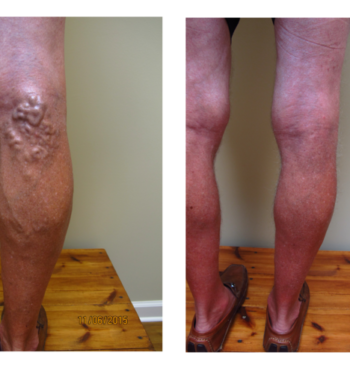
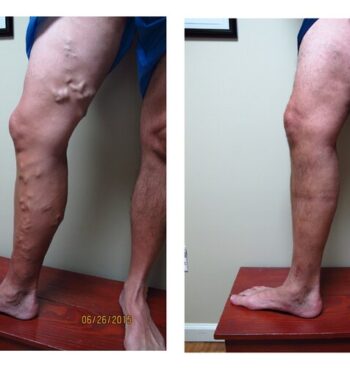
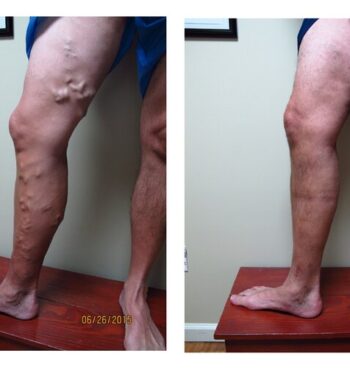
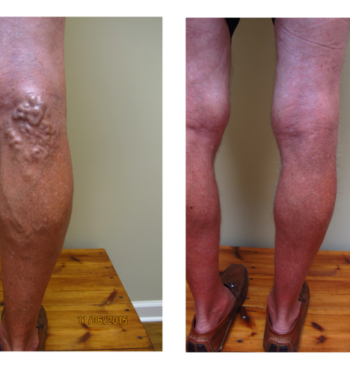
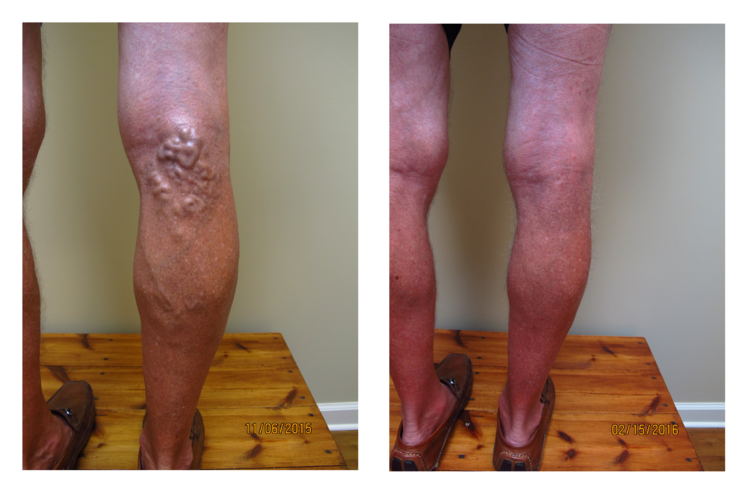
Varicose veins are abnormal, big blue bulging leg veins. They arise from leaky valves in the superficial venous system. Varicose veins can develop at any age and tend to get worse over time. They develop more commonly in women and may have some hormonal component. There are also genetic factors at work. Most people with varicose veins experience symptoms which may include: aching, a full heavy sensation, throbbing, tingling, itching, warmth, or swelling. If left untreated, varicose veins can cause brown staining called hemosiderin deposition, white patches called atrophie blanche, or flaking itchy skin called stasis dermatitis. If allowed to progress further patients may develop stasis ulcers or bleeding.
For decades, doctors have ignored varicose veins, but varicose veins are much more than a cosmetic issue. It is clear that they can cause significant symptoms and they are most definitely disfiguring. Modern treatments are effective at eliminating symptoms, restoring function, and improving body image.
Do not be embarrassed about showing your legs to your doctor. If you see your legs in any of our pictures feel free to call for an appointment. Varicose veins are common, curable, and treatments are covered by insurance and Medicare. If your legs look like any of the legs in our pictures please call us, we can help you.
Varicose Vein Treatment Options:
- Graded compression hose
- Sclerotherapy
- Endovenous laser ablation (ELAS/EVLT)
- Micro-phlebectomy
- Ultrasound guided sclerotherapy
- Combination of treatments
Venogram
A venogram is a minimally invasive procedure that is used in cases of venous obstruction. This procedure is performed with a small catheter that is inserted into a vein and then contrast (“dye”) is injected to map the veins and reveal the extent of the blockage. Additionally, the surgeon uses intravascular ultrasound (IVUS) and a state-of-the-art digital flat panel C-arm that gives hospital quality x-ray images. Then, the surgeon works to clear the obstruction with sophisticated catheters, wires, balloons, and stents. During the procedure, patients are lightly sedated and comfortable. When the procedure is over, patients are recovered in our office and go home within 1-2 hours.
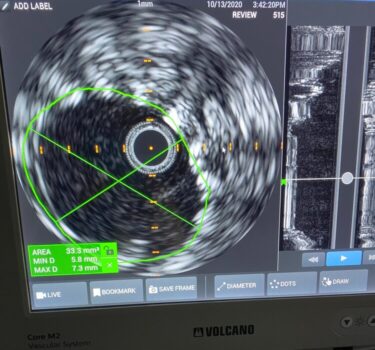
What is Pelvic Congestion Syndrome?
Chronic pelvic pain is common, particularly among women. In fact, 39% of women in the United States will report experiencing pelvic pain at some point in their lifetimes. This represents a large proportion of visits to OBGYNs and is a common reason that women undergo laparoscopic surgery and/or hysterectomy (removal of the uterus). While there are many causes of female pelvic pain, this complaint may be due to an underlying venous disorder, known as Pelvic Venous Compression. Pelvic Venous Compression (formerly, “Pelvic Congestion Syndrome”) is a common and often unrecognized condition affecting men and women. Patients with Pelvic Venous Compression often complain of pelvic heaviness, bloating, pain with sexual intimacy, pain with urination and bowel movements, and varicose veins in the groin. For many years there were few treatments for Pelvic Venous Compression, but there are now several minimally invasive procedures for this debilitating condition. Drs. Tapper and Diamond are well-versed in the diagnosis and management of Pelvic Venous Compression and are able to provide several therapeutic options in the outpatient setting.
Treatment Options
- Outpatient Diagnostic Venography
- Intravascular Ultrasound
- Venous Embolization
- Surgical Treatment
Vascular Ultrasound
Drs. Tapper and Diamond are both Registered Physicians in Vascular Interpretation, holding a specialized advanced certification in reading vascular ultrasounds. Each has extensive experience in interpreting ultrasound data to provide an accurate diagnosis of venous disorders.
Additionally, both use ultrasound to identify compromised veins that may be leading to ulcers or wounds of the lower leg. Often, these veins can be treated with a simple injection that is nearly painless and is performed right in our office. These injections are very effective, do not require anesthesia and are very effective in the treatment of ulceration.
Dr. Tapper and Dr. Diamond will diagnose and treat:
- Varicose Veins
- Deep Venous Thrombosis (DVT)
- Superficial Thrombophlebitis
- Hyper-coagulable States
- Post-phlebitic syndrome
- Stasis ulcers
- Lymphedema
Micro-Phlebectomy
Phlebectomy is used to remove veins that are too big for sclerotherapy. Before the procedure, you will be given antibiotics, non‐narcotic pain pills, and Valium for relaxation. Your veins will be outlined with a magic marker and photographed.
The area over the marked veins will be injected with local anesthesia. The injection of anesthetic hurts for a few seconds but then the area goes numb. Once the area is numb, very small (1/8 to 1/4–inch) incisions are made and the veins are removed. The incisions are closed with Steri-Strip; no sutures are required. The small incisions heal very nicely and are hardly visible after a year.
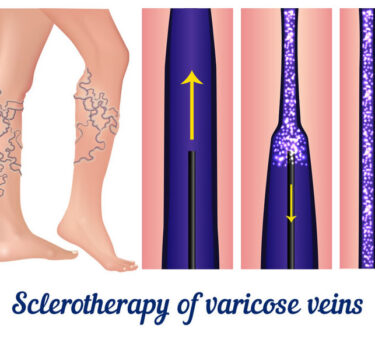
Sclerotherapy
Sclerotherapy is the injection of a Solution into abnormal veins using a small pediatric needle. The solution does not hurt, yet it irritates the inside lining of the vein which causes the vein to collapse or sclerose. Sclerotherapy is performed on spider veins, Telangiectasias, and small varicose veins. Sclerotherapy is a simple and ingenious concept, but its proper execution is an art that can take years to master. Sclerotherapy causes the targeted vein to destroying itself without damaging the surrounding tissue
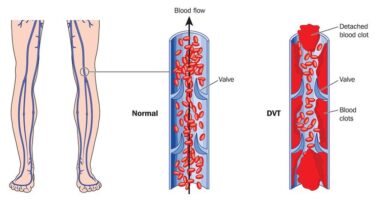
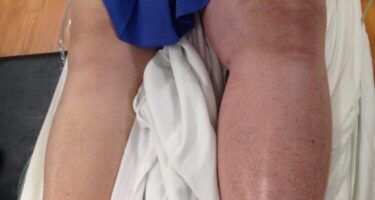
Deep Venous Thrombosis (DVT)
Deep Venous Thrombosis (DVT) is one of the few dangerous venous diseases. DVT is a major clot in a deep intra-muscular leg vein. It usually presents as swelling and pain in the affected limb. Although one can get DVT in pelvic, chest, neck, and arm veins it is most commonly diagnosed in the legs. The immediate danger is that the clot can break off and go to the heart and lungs. This event is called a pulmonary embolus and can be fatal.
The treatment for DVT involves anticoagulation or blood thinners. There are a variety of medications that can be used, but the key is to stop the clot from progressing. Sometimes the clot is so extensive that “clot buster” or tPA is used to dissolve it. This is a minimally invasive procedure performed by Dr. Tapper and Dr. Diamond in the hospital. The idea is to dissolve the clot before it damages the delicate valves in the deep veins. The sooner a clot is dissolved, the better the chance for normal vein valve function.
Major stimuli for clot formation include immobility (such as plane flight or long car ride), trauma, cancer, genetic conditions, and certain drugs. If you experience sudden onset of pain and swelling in your calf or thigh in such a setting, call your doctor, you may have a DVT.
Superficial Thrombophlebitis
Sometimes people develop a painful hard knot in the leg which may actually be a clot in a superficial vein. This problem is called superficial thrombophlebitis or STP.
It is painful, warm, red, and very tender. STP is best treated with NSAIDs (nonsteroidal anti-inflammatory drugs like aspirin and ibuprofen), along with warm compresses. Sometimes blood thinners are required if the clot is extensive. Emergency rooms and walk-in clinics often prescribe antibiotics, which are unnecessary as there is no infection. The redness associated with phlebitis is due to the intense inflammatory response to the clot. This response is blunted by NSAIDs and will dissipate in a few days.
SYMMETRY VASCULAR CENTER IS PROUD TO OFFER TREATMENT FOR PATIENTS IN OKEECHOBEE FOR PATIENTS WITH ARTERIAL DISEASE
CONFUSED ABOUT YOUR VASCULAR ISSUES?
Call us or setup an appointment to come in and discuss your options with one of our expert doctors or qualified staff members.
Designed by Tatem Web Design LLC.